What should I do if my 6-year-old child has astigmatism?
Astigmatism not only impairs visual acuity but also causes significant inconvenience in daily life. If left untreated, the condition may progressively worsen—increasing treatment complexity and raising the risk of other ocular diseases, even blindness. What should be done for a 6-year-old child with astigmatism?
Management of Astigmatism in 6-Year-Old Children
For 6-year-old children diagnosed with astigmatism, management depends on the degree of refractive error and may involve corrective eyewear or observation alone. Astigmatism arises from asymmetry in the corneal meridians, causing incoming light rays to focus at multiple points rather than a single point—a phenomenon known as “astigmatic blur.” Clinically, most children have mild astigmatism without obvious symptoms or reduced visual acuity, thus requiring no specific intervention. However, if astigmatism exceeds 100 diopters (D) and is accompanied by decreased vision, cycloplegic refraction is essential to obtain an accurate assessment of refractive status. Special vigilance is warranted when visual development lags behind age-appropriate norms and high astigmatism is present, as this increases the risk of amblyopia. In such cases, corrective glasses are indicated to optimize optical input; early spectacle wear combined with active amblyopia therapy (e.g., patching or visual training) significantly improves visual outcomes. Therefore, mild astigmatism in 6-year-olds generally does not require treatment, whereas astigmatism exceeding 100 D warrants spectacle correction based on visual function.
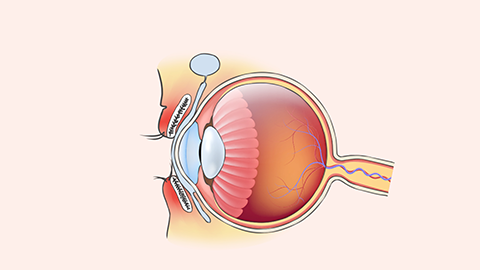
In 6-year-old children presenting with astigmatism, it is crucial to rule out underlying organic eye disease—including corneal opacities (e.g., leukoma), corneal tumors, intraocular tumors, congenital cataracts, or congenital glaucoma. In the absence of structural pathology, refined refraction should be performed to determine whether the astigmatism originates from the cornea, lens, or other ocular structures. Most pediatric astigmatism is regular and attributable to corneal irregularity, necessitating correction via refraction and spectacles. Nevertheless, for astigmatism exceeding 300 D, additional evaluation—including corneal topography—is recommended to exclude keratoconus and enable early diagnosis and intervention.

Patients should cultivate healthy visual habits and maintain good ocular hygiene: avoid reading or using mobile devices while lying down, and adopt proper posture during near work. Additionally, children should engage in ample outdoor activities and minimize prolonged near-vision tasks. We hope this information proves helpful.




