Is it necessary to extract wisdom teeth?
Generally speaking, not all wisdom teeth require extraction. The decision to extract should be based on a comprehensive assessment of the tooth’s position, occlusion, and overall oral health. A detailed analysis follows:
If a wisdom tooth has fully erupted, is properly aligned, establishes normal occlusion with its opposing tooth, is easily accessible for daily cleaning, shows no history of recurrent inflammation or gingival pain and swelling, does not impinge upon adjacent teeth or cause food impaction, does not interfere with occlusion or masticatory function, and exhibits no caries or periodontal disease, such a wisdom tooth may be retained without indication for extraction.
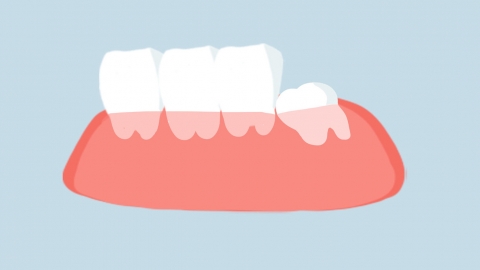
Conversely, if a wisdom tooth is impacted or malpositioned—such as partially erupted or angled—it may trap debris and bacteria, predisposing to recurrent pericoronitis and gingival inflammation, redness, and pain. It may also exert pressure on adjacent teeth, leading to increased interdental spacing, caries in neighboring teeth, and alveolar bone resorption. Additionally, if the opposing tooth is missing—causing the wisdom tooth to over-erupt and disrupt occlusion—or if extraction is indicated for orthodontic treatment (e.g., to prevent dental crowding) or to alleviate temporomandibular joint discomfort, early removal is recommended to prevent more serious oral complications.
To accurately assess whether a wisdom tooth should be retained, it is advisable to consult a reputable dental clinic for radiographic imaging (e.g., panoramic X-ray or CBCT). A qualified dentist will evaluate root morphology and eruption direction and provide an evidence-based, individualized treatment plan—rather than retaining or extracting the tooth arbitrarily or without professional guidance.




