What is the treatment for Henoch-Schönlein purpura?
Allergic purpura may be triggered by food allergies, drug allergies, compromised immunity, allergic vasculitis, or systemic lupus erythematosus (SLE), and treatment should be tailored according to the underlying cause. Prompt medical consultation is strongly recommended, and therapy should be conducted under the guidance of a qualified physician.
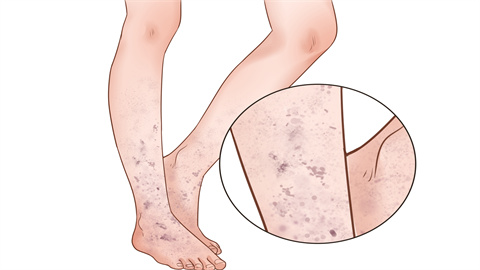
1. Food Allergy
Certain foods—such as seafood, milk, eggs, and legumes—may trigger allergic purpura. The immune system mistakenly identifies these substances as harmful foreign agents, initiating an immune response that leads to antibody production, vascular inflammation, and subsequently, purpura. Typical manifestations include cutaneous purpura, often accompanied by abdominal pain and arthralgia. Identifying potential allergens—possibly via allergen testing—and strictly avoiding ingestion of foods containing the identified allergen are essential steps in management.
2. Drug Allergy
Some medications—including penicillin, sulfonamides, and antipyretic-analgesics—can also induce allergic purpura. Upon entering the body, these drugs act as haptens, binding to endogenous proteins to form complete antigens. This triggers an immune response, resulting in inflammation and purpuric lesions. If drug allergy is suspected as the cause, the offending medication must be discontinued immediately. During medical evaluation, patients should inform their physician of any prior drug allergies to facilitate selection of appropriate alternative therapies.
3. Compromised Immunity
Reduced immune function increases susceptibility to infections caused by bacteria, viruses, or parasites, which may precipitate allergic purpura. Such infections stimulate abnormal immune responses, leading to vascular inflammation and damage, and ultimately, purpura. Preventive measures—including infection avoidance, strict personal hygiene, frequent handwashing, and minimizing exposure to crowded places—especially during peak influenza season—are crucial.
4. Allergic Vasculitis
This is an inflammatory disorder primarily affecting small blood vessels. Immune complexes deposit within the walls of small vessels, activating the complement system and provoking vascular inflammation. Consequently, vascular permeability increases, allowing red blood cells to extravasate and form purpuric lesions. In addition to skin purpura, patients may experience fever, fatigue, and arthralgia. Under physician supervision, medications such as enteric-coated aspirin tablets, colchicine tablets, and methylprednisolone tablets may be prescribed to alleviate symptoms.
5. Systemic Lupus Erythematosus (SLE)
SLE is an autoimmune disease in which the immune system erroneously attacks the body’s own tissues and organs. When small vessels are involved, clinical features resembling allergic purpura may occur—including cutaneous purpura, joint pain, and oral ulcers. Treatment should follow physician recommendations and may include medications such as danazol capsules, methylprednisolone tablets, and tripterygium glycosides tablets to relieve symptoms.





