What Causes Vaginal Burning Pain?
Vaginal burning sensation is commonly caused by unsafe sexual practices or unhygienic lifestyle habits. But what causes vaginal burning pain?
What Causes Vaginal Burning Pain?
Vaginal burning pain is primarily attributable to gynecological inflammatory infections, such as bacterial vaginosis, fungal (candidal) vaginitis, trichomoniasis, urinary tract infections, and cervical inflammation. In women, vaginal burning pain may indicate underlying inflammation, which can lead to abnormal vaginal discharge that repeatedly irritates the vaginal mucosa, resulting in a burning sensation. Malignant tumors compressing tissues within the vaginal wall may also cause burning pain. In married women, vigorous sexual intercourse may excessively stimulate vaginal wall tissues, leading to burning pain. When experiencing vaginal burning pain, patients should seek medical evaluation at a hospital for gynecological examination, vaginal discharge analysis, and cervical screening. These tests help determine whether vaginal inflammation is present, identify its specific type, assess for cervical lesions or vaginal trauma, and guide appropriate, etiology-based treatment.
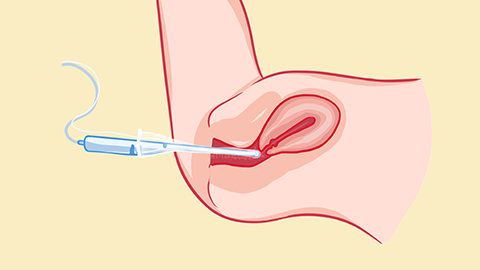
Vaginal warmth or heat sensation typically results from the entry of bacteria, trichomonads, or other pathogens into the vagina due to unsafe sexual practices or poor hygiene. Clinically, this symptom is frequently associated with conditions such as vaginitis, cervicitis, and genital warts.
Vaginitis: Under physician guidance, patients may take oral metronidazole or tinidazole. For candidal vaginitis, fluconazole is commonly prescribed. Patients with atrophic vaginitis may receive hormonal therapy, such as estradiol valerate.
Cervicitis: Antibiotics such as azithromycin or levofloxacin may be prescribed to reduce inflammation.
Avoid scratching the vaginal area with your hands to prevent skin abrasions and subsequent worsening of infection and burning pain. Each evening before bed, gently cleanse the external genitalia with warm water to maintain cleanliness. We hope this article has been helpful. Wishing you a happy life and good health!




