How is endometritis caused?
Generally, endometritis is caused by bacterial invasion due to poor menstrual hygiene, decreased estrogen levels leading to weakened mucosal resistance, vaginitis, cervicitis, or submucosal uterine fibroids. It is recommended to seek timely medical attention, identify the underlying cause, and undergo symptomatic treatment under a doctor's guidance. Detailed analysis is as follows:
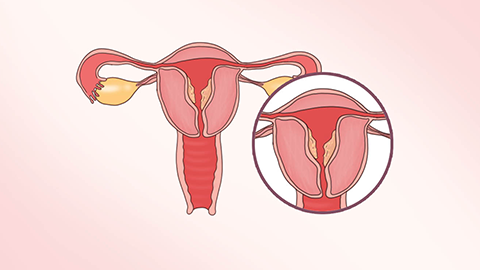
1. Bacterial invasion due to poor menstrual hygiene: During menstruation, the endometrium sheds and forms wounds. If unclean sanitary pads are used, or if a woman takes baths or engages in sexual activity during menstruation, bacteria can easily enter the uterine cavity and cause inflammation, accompanied by foul-smelling menstrual blood and mild lower abdominal pain, with symptoms possibly worsening after menstruation ends. It is important to change sanitary pads frequently during menstruation, avoid tub baths and sexual activity, and clean the vulva with warm water to maintain hygiene and reduce bacterial growth and invasion.
2. Weakened mucosal resistance due to decreased estrogen levels: Postmenopausal women experience reduced estrogen secretion, leading to thinning of the endometrium and decreased mucosal resistance, making it easier for bacterial infection to cause inflammation. Symptoms include vaginal dryness, increased secretions, and slower recovery after infection. Maintain vulvar moisture and avoid using irritating cleansers. If necessary, apply estrogen cream locally under a doctor's guidance to enhance mucosal resistance. Wear loose cotton underwear daily to reduce mucosal friction injuries.
3. Vaginitis: Inflammation caused by bacterial or fungal infections in the vagina can allow pathogens to ascend and affect the endometrium, causing endometritis, accompanied by vaginal itching and abnormal secretions. Recurrent vaginitis can easily trigger endometrial inflammation. Avoid scratching the vagina, follow medical advice to treat vaginitis with medications such as metronidazole suppositories, clotrimazole vaginal tablets, or tinidazole suppositories, and have regular follow-ups after inflammation control to prevent ascending infection of the endometrium.
4. Cervicitis: Inflammation caused by chlamydia, mycoplasma, or other infections in the cervix allows pathogens to breach the cervical barrier and enter the uterine cavity, causing endometritis, accompanied by cervical congestion, contact bleeding, and mucopurulent secretions. Avoid unhygienic sexual activity and reduce cervical irritation. Follow medical advice to treat cervicitis with medications such as azithromycin capsules, doxycycline hydrochloride tablets, or cefixime capsules to prevent pathogen ascent. Treat sexual partners simultaneously to avoid cross-infection.
5. Submucosal uterine fibroids: Fibroids protruding into the uterine cavity can cause mucosal friction and damage, allowing bacteria to invade and cause infection, resulting in endometritis, accompanied by increased menstrual flow, prolonged periods, and foul-smelling secretions. During infection, bed rest is recommended to reduce fibroid friction. Follow medical advice to control infection with medications such as levofloxacin tablets, clindamycin capsules, or metronidazole tablets. After infection subsides, undergo hysteroscopic fibroid removal to reduce mucosal damage and infection risk.
Maintain a regular lifestyle to enhance immune function and reduce infection risk. Eat light meals and consume more fruits and vegetables rich in vitamin C to promote mucosal repair. Avoid frequent intrauterine procedures to reduce endometrial injury and lower inflammation risk. Undergo regular gynecological checkups to detect reproductive system inflammation early and treat it promptly, preventing involvement of the endometrium.





