How is ankylosing spondylitis diagnosed?
As lifestyles evolve, various diseases have emerged—including ankylosing spondylitis. So, how is ankylosing spondylitis diagnosed?
How Is Ankylosing Spondylitis Diagnosed?
Diagnosis of ankylosing spondylitis primarily relies on three aspects: first, the patient’s clinical symptoms; second, positive physical examination findings; and third, imaging studies combined with HLA-B27 testing as an auxiliary diagnostic tool. Treatment options include massage therapy, physiotherapy, needle-knife therapy, endothermal needle therapy, and silver needle therapy. The mainstay pharmacological treatment consists of nonsteroidal anti-inflammatory drugs (NSAIDs).
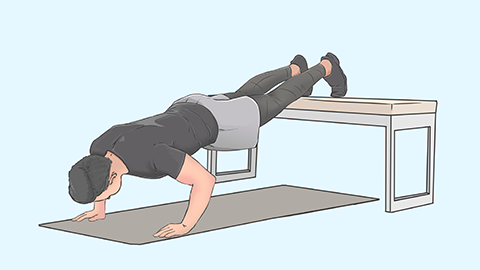
First, patients with ankylosing spondylitis typically present with inflammatory low back pain—characterized by onset before age 40. Symptoms usually worsen after prolonged sitting, do not improve with rest, but ease with physical activity. Positive physical signs include restricted lumbar mobility, often accompanied by reduced chest expansion. Imaging studies reveal inflammatory changes in the sacroiliac joints, such as joint space narrowing and subchondral bone sclerosis. A positive HLA-B27 test further supports the diagnosis of ankylosing spondylitis. Collectively, these features contribute to establishing the diagnosis.
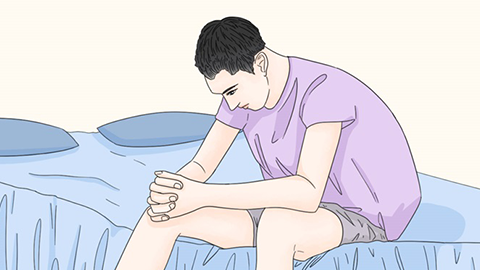
Patients with ankylosing spondylitis should pay close attention to daily lifestyle habits. Generally, patients require enhanced nursing care, regular physical exercise, correction of poor posture, cultivation of healthy living habits, maintenance of a positive emotional state, and strict adherence to prescribed medications. Diet should be light and nutritionally balanced—avoiding picky eating, overeating, or binge eating. We hope this information proves helpful!








