What are acute and chronic glomerulonephritis?
Acute and chronic glomerulonephritis is a condition commonly seen in older adults, with symptoms ranging from mild to severe. So, what exactly is acute and chronic glomerulonephritis?
What Is Acute and Chronic Glomerulonephritis?
Acute glomerulonephritis most frequently occurs following a streptococcal infection. It has an abrupt onset, presenting with sudden hematuria, proteinuria, edema, and hypertension—sometimes accompanied by transient renal insufficiency. Histopathologically, it commonly manifests as proliferative glomerulonephritis affecting the capillaries. Acute glomerulonephritis is typically self-limiting; management generally involves rest and symptomatic treatment, and most patients recover spontaneously.
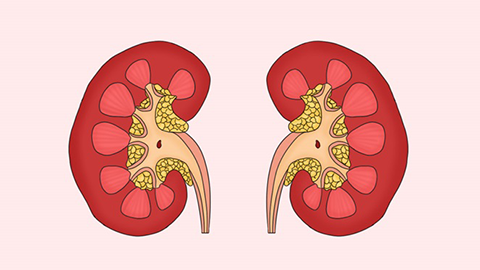
The hallmark clinical features of chronic glomerulonephritis include proteinuria, hematuria, hypertension, and edema. Its onset varies, the disease course is protracted, progression is slow, and varying degrees of renal insufficiency may develop over time, ultimately leading to chronic renal failure. Histopathologically, chronic glomerulonephritis encompasses several subtypes, including mesangial proliferative glomerulonephritis, membranoproliferative glomerulonephritis, focal segmental glomerulosclerosis, and others.
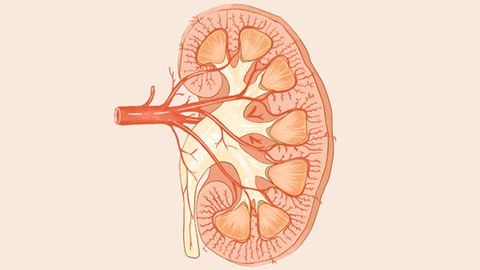
In general, chronic glomerulonephritis is a slowly progressive chronic disease that ultimately results in renal failure. Acute nephritis includes acute glomerulonephritis, rapidly progressive glomerulonephritis, and acute interstitial nephritis. Acute glomerulonephritis—when uncomplicated by renal failure or infection—is self-limiting and usually resolves spontaneously. Patients should prioritize rest and undergo regular monitoring. Nevertheless, acute glomerulonephritis remains a serious condition. We hope this information is helpful to you.










